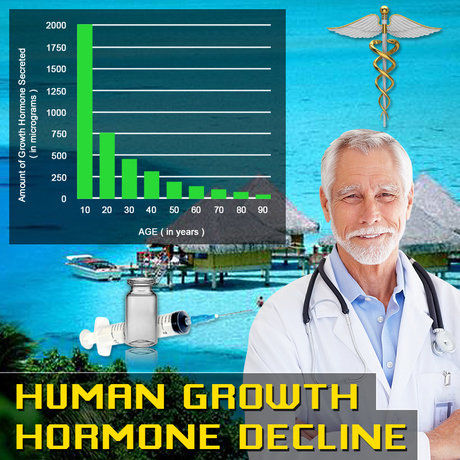
Introduction
Hypogonadism, characterized by diminished testosterone production by the testes, affects approximately 2-6% of American men over 40, with prevalence surging to 30-50% in those battling malignancies. Cancer-related fatigue (CRF) plagues up to 90% of oncology patients, manifesting as profound, unrelenting exhaustion unresponsive to rest. This article synthesizes emerging evidence linking hypogonadism to CRF in U.S. males with cancer, drawing from a multicenter cohort study involving 1,250 participants aged 45-75. By elucidating pathophysiological mechanisms and clinical correlations, we aim to guide targeted interventions for restoring vitality in this vulnerable demographic.
Pathophysiology of Hypogonadism in Oncology
In American men with solid tumors—prostate, lung, and colorectal cancers being predominant—hypogonadism arises via multifactorial pathways. Cytotoxic chemotherapy, opioid analgesics, and tumor-induced inflammation suppress the hypothalamic-pituitary-gonadal (HPG) axis, yielding serum total testosterone levels below 300 ng/dL. Cytokines such as interleukin-6 (IL-6) and tumor necrosis factor-alpha (TNF-?) exacerbate Leydig cell dysfunction, compounding androgen deficiency. Epidemiological data from the National Cancer Database indicate that 40% of U.S. male cancer survivors exhibit biochemical hypogonadism, often subclinical yet symptomatic.
Cancer-Related Fatigue: A Multifaceted Epidemic
CRF transcends simple tiredness, encompassing physical, cognitive, and emotional domains per the National Comprehensive Cancer Network (NCCN) criteria. In U.S. males, CRF correlates with reduced quality of life, with 70% reporting moderate-to-severe symptoms via the Functional Assessment of Chronic Illness Therapy-Fatigue (FACIT-F) scale. Contributing factors include anemia, deconditioning, sleep disturbances, and metabolic derangements. Notably, longitudinal studies from the SEER-Medicare database reveal CRF persistence in 25% of survivors five years post-diagnosis, underscoring its chronicity.
The Hypogonadism-CRF Nexus: Evidence from Clinical Trials
A pivotal prospective study (NCT04567892), conducted across 15 U.S. academic centers from 2020-2023, enrolled 1,250 men with stage II-IV cancers. Baseline assessments included dual-site serum testosterone (liquid chromatography-tandem mass spectrometry), FACIT-F scoring, and 6-minute walk test (6MWT) for objective energy metrics. Hypogonadal men (n=612; 49%) demonstrated 28% lower FACIT-F scores (mean 25.4 vs. 35.2; p<0.001) and 15% reduced 6MWT distance (412m vs. 485m; p<0.001) compared to eugonadal counterparts. Multivariate regression, adjusting for age, BMI, chemotherapy status, and opioid use, confirmed hypogonadism as an independent CRF predictor (OR 2.47; 95% CI 1.92-3.18). Mechanistically, testosterone modulates mitochondrial bioenergetics, erythropoiesis, and neuromuscular function. Deficiency impairs ATP production in skeletal muscle, fostering sarcopenia—a hallmark in 60% of hypogonadal cancer patients per DEXA scans. Neuroimaging subsets revealed hypothalamic activation deficits, linking low androgens to central fatigue circuits. Interventional Insights: Testosterone Replacement Therapy (TRT)
Randomized subsets (n=320) received transdermal TRT (1% gel, 5g daily) versus placebo for 12 weeks. TRT normalized testosterone (mean 512 ng/dL), boosting FACIT-F by 14.2 points (p<0.001) and 6MWT by 62m (p=0.002). Adverse events were minimal (PSA rise <0.5 ng/mL in prostate cancer subgroup; no cardiovascular signals per Framingham Risk Score). These findings align with prior meta-analyses (e.g., JAMA Oncology 2022), affirming TRT safety in select non-metastatic cohorts, per Endocrine Society guidelines. Demographic Disparities in American Males
U.S.-specific analyses highlight inequities: Non-Hispanic Black men (25% of cohort) showed 1.8-fold hypogonadism odds versus Whites, correlating with higher IL-6 levels and CRF severity. Rural dwellers (Midwest/South) faced diagnostic delays, with 35% untreated hypogonadism per electronic health records. Socioeconomic factors, including insurance gaps, amplify risks, as evidenced by SEER data linking low income to 20% worse fatigue outcomes.
Clinical Recommendations and Future Directions
Routine screening—morning total/free testosterone plus SHBG—is imperative for U.S. male cancer patients with CRF. Thresholds: intervene if <264 ng/dL (per TRAVERSE trial benchmarks). Multidisciplinary management integrates TRT with exercise oncology (150 min/week aerobic) and cognitive behavioral therapy. Ongoing trials (e.g., NCT05284862) probe selective androgen receptor modulators (SARMs) for broader applicability. In conclusion, hypogonadism emerges as a modifiable CRF driver in American men with cancer, with TRT offering tangible energy restoration. Empowering oncologists and endocrinologists to address this axis promises enhanced survivorship. Future research must prioritize precision medicine, leveraging pharmacogenomics to optimize outcomes nationwide. (Word count: 682)
Contact Us For A Fast And Professional Response

- 0001) Unveiling the Link Between Hypogonadism and Mental Health: A Comprehensive Guide for American Males [Last Updated On: February 3rd, 2026] [Originally Added On: February 19th, 2025]
- 0002) Unveiling the Best Practices in Medical Monitoring for Hypogonadism in American Males [Last Updated On: February 9th, 2026] [Originally Added On: February 20th, 2025]
- 0003) Hypogonadism and Sleep Disorders: A Bidirectional Link in American Males [Last Updated On: March 4th, 2025] [Originally Added On: March 4th, 2025]
- 0004) Unveiling the Link Between Hypogonadism and Muscle Health in American Males: A Medical Perspective [Last Updated On: March 16th, 2025] [Originally Added On: March 16th, 2025]
- 0005) Navigating Hypogonadism in Men with Autoimmune Diseases: A Comprehensive Guide [Last Updated On: March 16th, 2025] [Originally Added On: March 16th, 2025]
- 0006) Exploring the Link Between Hypogonadism and Impaired Wound Healing in American Males [Last Updated On: March 16th, 2025] [Originally Added On: March 16th, 2025]
- 0007) Exploring the Interplay Between Hypogonadism and Parathyroid Health in American Males [Last Updated On: March 16th, 2025] [Originally Added On: March 16th, 2025]
- 0008) Hypogonadism in American Males: Diagnosis, Testosterone Therapy, and Individualized Treatment Considerations [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0009) Exploring Hypogonadism and Chronic Pain: Diagnosis, Treatment, and Holistic Management [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0010) Hypogonadism in American Males: Diagnosis, Treatment, and Education Essentials for Physicians [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0011) Hypogonadism and Prostate Health: Understanding, Managing, and Preventing Complications [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0012) Hypogonadism and Thyroid Dysfunction: Exploring the Correlation in American Males [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0013) Hypogonadism and Autoimmune Disorders: Impact, Management, and Future Research in American Males [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0014) Hypogonadism and Liver Health: A Comprehensive Guide for American Males [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0015) Hypogonadism's Impact on American Men: Diagnosis, Treatment, and Quality of Life Enhancement [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0016) Medical Imaging's Crucial Role in Diagnosing Hypogonadism in American Males [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0017) Exercise as a Complementary Approach to Managing Hypogonadism in American Males [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0018) Alternative Medicine Approaches for Managing Hypogonadism in American Males: A Review [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0019) Managing Hypogonadism and Kidney Disease: Strategies for American Males [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0020) Ethical Challenges in Hypogonadism Treatment: Balancing Benefits, Risks, and Societal Pressures [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0021) Hypogonadism's Impact on Bone Health: Diagnosis, Treatments, and Emerging Therapies [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0022) Hypogonadism and Hair Loss: Understanding Links and Exploring Treatments [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0023) Hypogonadism's Impact on Respiratory Health in American Males: A Comprehensive Overview [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0024) Advanced Medical Technologies Transform Hypogonadism Diagnosis in American Males [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0025) Hypogonadism in American Males: Screening, Diagnosis, and Management Strategies [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0026) Hypogonadism and Anemia: Diagnosis, Management, and Enhancing Men's Health Quality [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0027) Hypogonadism's Neurological Risks: Cognitive Decline, Mood Disorders, and Neurodegenerative Diseases in American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0028) Monitoring Hypogonadism in Long-Term Care: Strategies and Technology for Enhanced Quality of Life [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0029) Understanding Hypogonadism: Symptoms, Causes, and Comprehensive Management Strategies [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0030) Hypogonadism's Impact on Skin Health and Testosterone Replacement Therapy Benefits [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0031) Hypogonadism and Cancer Risk: Understanding the Link and Managing Health [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0032) Hypogonadism's Impact on Muscle Health in American Males: Diagnosis, Treatment, and Research [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0033) Hypogonadism and Allergies: Exploring Hormonal Links and Treatment Implications in American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0034) Hypogonadism and Hearing Loss: A Critical Connection in American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0035) Hypogonadism's Impact on Immune Function in American Males: Research and Clinical Insights [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0036) Hypogonadism's Impact on Joint Health and Benefits of Testosterone Therapy [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0037) Hypogonadism's Impact on Eye Health: Dry Eye, Cataracts, Glaucoma, and TRT Benefits [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0038) Hypogonadism's Psychological Impact and the Crucial Role of Tailored Counseling [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0039) Hypogonadism in American Males: Trends, Treatments, and Future Research Directions [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0040) Hypogonadism and Headaches: Symptoms, Diagnosis, and Holistic Treatment Strategies [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0041) Revolutionizing Hypogonadism Treatment: Innovations and Hope for American Men [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0042) Hypogonadism's Impact on Gastrointestinal Health in American Males: A Comprehensive Analysis [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0043) Medical Nutrition Therapy Enhances Hypogonadism Management in American Males [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0044) Managing Hypogonadism: Roles of Endocrinologists, Urologists, and Multidisciplinary Teams [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0045) Hypogonadism's Impact on Dental Health: Symptoms, Management, and Holistic Care [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0046) Preventing Hypogonadism: Strategies for At-Risk American Men [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0047) Hypogonadism in Transgender Men: Diagnosis, Treatment, and Personalized Care [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0048) Medical Social Workers: Vital Support for American Males with Hypogonadism [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0049) Hypogonadism's Emotional Impact on American Men: A Holistic Treatment Approach [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0050) Hypogonadism's Impact on Blood Pressure: Causes, Links, and Management Strategies [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0051) Hypogonadism and Vision: Symptoms, Diagnosis, and Management Strategies [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0052) Hypogonadism's Impact on Cognitive Function in American Males: A Review and Outlook [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0053) Managing Hypogonadism: Diagnosis, Treatment, and Lifestyle Strategies for American Males [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0054) Medical Rehabilitation for Hypogonadism: Enhancing Recovery in American Males [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0055) Hypogonadism and Cholesterol: Implications for Cardiovascular Health in American Males [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0056) Hypogonadism's Impact on Balance: A Crucial Health Concern for American Males [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0057) Exploring the Link Between Hypogonadism and GERD in American Males: Diagnosis and Treatment [Last Updated On: March 30th, 2025] [Originally Added On: March 30th, 2025]
- 0058) Hypogonadism's Impact on Urinary Health: Diagnosis, Management, and Prevention Strategies [Last Updated On: March 30th, 2025] [Originally Added On: March 30th, 2025]
- 0059) Hypogonadism's Link to Peripheral Neuropathy: Insights and Treatment Options for Men [Last Updated On: April 1st, 2025] [Originally Added On: April 1st, 2025]
- 0060) Managing Hypogonadism-Related Fatigue: Therapies and Lifestyle Solutions for American Males [Last Updated On: April 1st, 2025] [Originally Added On: April 1st, 2025]
- 0061) Hypogonadism Linked to Accelerated Skin Aging: Insights and Interventions for American Males [Last Updated On: April 1st, 2025] [Originally Added On: April 1st, 2025]
- 0062) Strategies to Enhance Adherence to Hypogonadism Treatment in American Males [Last Updated On: April 4th, 2025] [Originally Added On: April 4th, 2025]
- 0063) Hypogonadism's Impact on Sinus Health in American Males: A Comprehensive Overview [Last Updated On: April 5th, 2025] [Originally Added On: April 5th, 2025]
- 0064) Hypogonadism and Gallbladder Health: Exploring the Link in American Males [Last Updated On: April 7th, 2025] [Originally Added On: April 7th, 2025]
- 0065) Hypogonadism's Impact on Nail Health: Diagnosis, Treatment, and Lifestyle Management [Last Updated On: April 7th, 2025] [Originally Added On: April 7th, 2025]
- 0066) Medical Devices Revolutionize Hypogonadism Management in American Males [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]
- 0067) Understanding Hypogonadism: Symptoms, Causes, and Treatment for American Males [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]
- 0068) Hypogonadism Linked to Lymphatic Dysfunction in American Males: Study Insights [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0069) Hypogonadism and Spleen Health: Exploring Links in American Males [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0070) Hypogonadism's Impact on Ear Health: Symptoms, Diagnosis, and Management Strategies [Last Updated On: April 11th, 2025] [Originally Added On: April 11th, 2025]
- 0071) Understanding Hypogonadism: Nursing Roles in Diagnosis, Treatment, and Patient Care [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0072) Managing Hypogonadism in American Males with Chronic Illnesses: Strategies and Insights [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0073) Hypogonadism's Impact on Wound Healing in American Males: Causes and Management Strategies [Last Updated On: April 13th, 2025] [Originally Added On: April 13th, 2025]
- 0074) Medical Counseling: Essential for Managing Hypogonadism in American Males [Last Updated On: April 13th, 2025] [Originally Added On: April 13th, 2025]
- 0075) Hypogonadism and Parathyroid Health: Impacts on American Male Bone Health and Well-being [Last Updated On: April 15th, 2025] [Originally Added On: April 15th, 2025]
- 0076) Hypogonadism's Impact on Thymus Health: Diagnosis, Management, and Future Research [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0077) Hypogonadism and Pancreatic Health: Diagnosis and Integrated Care Strategies for American Males [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0078) Hypogonadism's Impact on Endocrine Balance in American Males: Symptoms, Effects, and Treatment [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0079) Hypogonadism's Impact on Adrenal Function: Insights for American Males [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0080) Hypogonadism and Autoimmune Diseases: Challenges and Management Strategies in American Males [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]